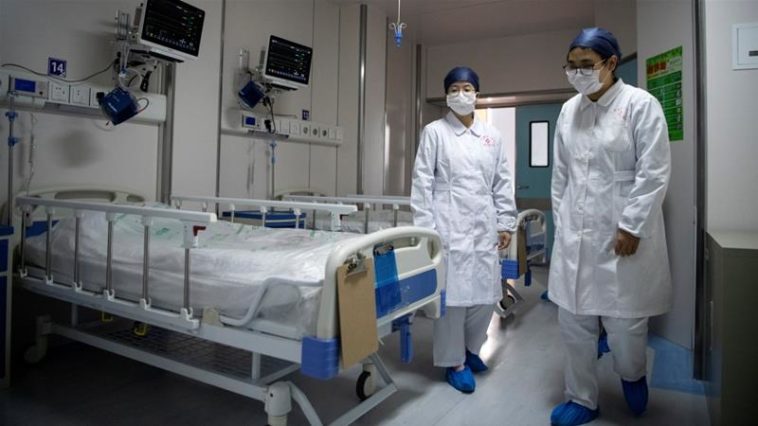
Some of the nurses that work at the Lawrence Hospital located in Bronxville, New York are being kept under the quarantine after it was identified that they had been exposed to the Coronavirus by an infected patient who had been treated at the hospital. So far in Washington, nearly 25 workers at the health care department have been kept under tight observation after they interacted with the people who were earlier not diagnosed with COVID-19 but later died due to the disease. As for Northern California, 3 of the healthcare workers have also been tested sportive for the Coronavirus while dozens of others have been kept in isolation.

The nature of the job of the healthcare workers puts them at high risk for contracting any such communicable diseases such as the COVID-19. Back in 2002 when the SARS outbreak occurred, nearly 1/5th of the total cases were identified among the healthcare workers. If the healthcare workers start to get sick in large numbers, it increases the pressure on the healthcare system which would have already been very high from the start of such an outbreak. This is why it is important that these healthcare workers have the proper access to all the protective equipment as well as are given the right authority to isolate the identified patients.

A nurse researcher as well as the director for the Institute for Biosecurity located at Saint Louis University, Terri Rebmann said, “Health care workers spend a lot of time up close with the patient doing high-risk activities.” These high-risk activities are the thing such as placing the serious patients on ventilators or collection of the sputum from the lungs of such patients.

PPE (Personal protective equipment) such as gloves, masks, and gowns are all the things that help the doctors and nurses remain safe while they treat the patients who are suffering from infectious diseases like the COVID-19. As per WHO (World Health Organization) and the CDC (Center For Disease Control and Prevention) has recommended to the healthcare systems that their health workers need to wear the N95 masks which is able to filter out the airborne particles as well as the tiny droplets that might have been coughed up by an infected patient.
Rebmann also says, “Most countries lack sufficient PPE to respond to a large scale event. That puts health care workers at risk.”

Healthcare workers are also at risk of contracting the COVID-19 disease if the infected patients are not identified promptly. If they are not identified early on, nurses and doctors might start to treat them without any necessary precaution which makes them susceptible to contracting an infection. Rebmann says, “It’s a risk not only to health care workers but to visitors and other patients at the hospital.” This is really concerning because the two patients who died in Washington were only diagnosed with COVID-19 after they died.

Rebmann says, “Not identifying someone who has a contagious disease is a concern. During the H1N1 epidemic, studies showed that if infected individuals weren’t identified, it was associated with staff exposure. The anxiety of knowing you might be at risk when you’re doing your job can be very challenging for health care workers. It’s physically and mentally draining.”

During the time of such outbreaks, workers of the healthcare system are putting their own personal safety at risk to take care of the others this is why leaving the mask on the shelves and following up the guidelines of public health is recommended for remaining safe from any viral infection. Not only does it keeps a person safe but also the ones that are working to keep others safe.
Related Content
Realme 6 and Realme 6 Pro have been announced for less than $200
First U.S. citizen’s death confirmed from Coronavirus in the Washington state
YouTube demonetizing Coronavirus videos and content creators are frustrated over this